- Home
- Employers
-
Members
-
Member Resources for Funding Advantage & Individual Advantage
>
- Explanation of Benefits for Funding Advantage Members
- Member FAQs
- Member-Hybrid >
- Member-Traditional >
- Member-Essentials >
- Member-PPO >
- Member-Cost Saver >
- Member-Minimum Essential Coverage >
- Member - Community Health Plan >
- Member-H&H PLan >
- Member-Vault PPO Resources >
- Member-Vault RBP >
- Member-Fundamental Care
- Member-Fundamental Care Value Plan
- Member Resources for Individual Advantage
- Benefit Extras >
- Self-Service Login >
- Find A Provider
- Prescription Benefits
- Member Download Forms >
-
Member Resources for Funding Advantage & Individual Advantage
>
-
Agents
- Provider
- About Us
- Contact Us
|
Telehealth, also called telemedicine, allows you to receive health care without an in-person visit to a provider by using computer, tablet or smartphone.
Telehealth technically started in the 1940s in Pennsylvania when providers realized they could send radiology images over the phone lines between two townships. In the 1950s, a Canadian doctor expanded on the concept and constructed a teleradiology system that was used in and around Montreal. And in 1967, the University of Miami School of Medicine partnered with a local fire department to transmit electrocardiographic rhythms over radio to Jackson Memorial Hospital in rescue situations.
9 Comments
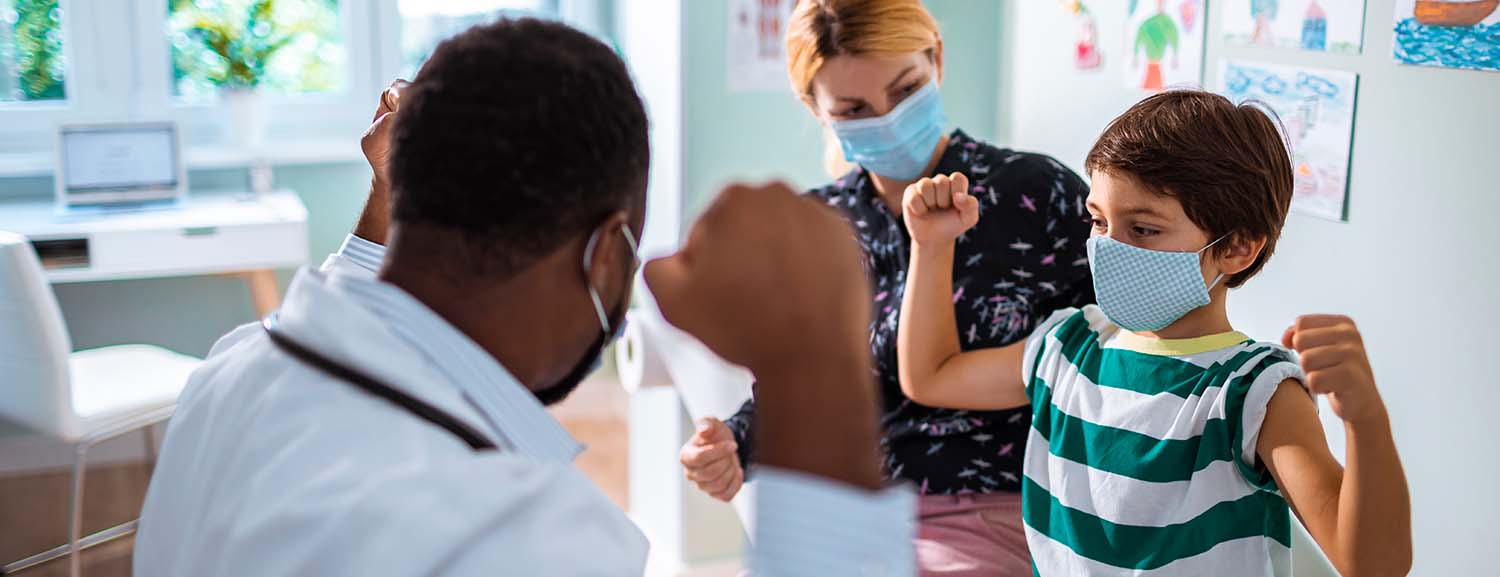
With the school year beginning, that means kids across the country are back to playing sports in middle school, high school and college. In addition to playing for their schools, some student athletes participate in club athletics over the course of the year.
As the parent of a student-athlete, you obviously know what’s best for them when it comes to their athletic careers and that includes being prepared for things like injuries in case the schools and athletic organizations don’t have medical coverage. It’s no wonder small businesses are confused when they are told they need to file Form 5500 with the Internal Revenue Service (IRS) and pay PCORI fees. For instance, if you look up 5500 filing requirements on the Internet, most sites say something like, “Form 5500 is required on behalf of any welfare benefit plan that has 100 or more participants as of the beginning of the plan year or is funded through a trust, regardless of participant count.”
Clear as mud to the average employer, right? WRONG! Let’s break it down. A minimum essential coverage (MEC) plan that doesn’t provide minimum value can still be an asset to large employers providing health coverage.
First, it helps to understand the definitions of minimum value and minimum essential coverage. Since 1949, May has been observed as Mental Health Awareness Month. It was established to increase awareness of the importance of mental health and wellness and to celebrate recovery from mental illness.
Telehealth is now playing a huge role in treating mental health and substance abuse. Telehealth is a covered benefit by many employer-based health plans as well as Medicare and Medicaid plans. Dreaming of retiring early? You’re not alone. The COVID-19 pandemic has forced many Americans to reevaluate their work-life balance.
Market research company Hearts and Wallets reports that about one in four Americans plan to retire before age 65 – a much higher percentage than in years past. If you’re one of the “one in four” and you think you’ve saved enough to retire early and cover your living expenses, there’s one more expense you should consider – health insurance. For many, the end of the year is a time to slow down, relax and reflect on the year behind us while setting resolutions for the year ahead. At Allied National, our employees are busy paying claims, providing agent support, closing new business and booking renewals. But we still have time to look back at what we accomplished in 2021 and share with our readers what’s ahead for Allied National in 2022. And be sure to take our quick survey at the end for a chance to win an Amazon gift card!
Direct Primary Care (DPC) is capturing the attention of employers who want to offer better health care coverage to their employees. With DPC, a patient can form a one-on-one relationship with their doctor and have 24/7 access to medical care. DPC has been shown to help provide superior healthcare for individuals, lowering their overall healthcare costs and improving outcomes.
The challenge for employers who want to offer DPC – how to ensure employees are covered for both primary care health services and care the DPC doctor can’t provide. Winter holidays are meant to be a joy-filled season with family and friends, but they also can bring a lot of stress. Here we are in 2021, with the continued risk of COVID-19 and its new variants still posing threats. In addition, now we have product and food supply shortages across the country – this sounds like a recipe for a higher-than-normal stress-filled holiday season.
The Affordable Care Act (ACA), also known as Obamacare, is a health care reform law that was enacted in March 2010. Some of the key goals of the ACA were to:
However, even though there are some “pros” to the Affordable Care Act, there are just as many “cons” for an ACA plan, many of which led to significantly higher health insurance premiums for individual and small employer health insurance. |
Welcome to the Allied BlogAllied NationalAllied National is a 90 Degree Benefits Company, a subsidiary of Blue Cross Blue Shield of Alabama. Founded in 1970, Allied National is one of the nation's oldest and most experienced third-party administrators. We're the small group benefit experts working to provide unique and affordable group health benefits to small business employers. Categories
All
|
|
© 2022 Allied National, LLC. All Rights Reserved.
|
- Home
- Employers
-
Members
-
Member Resources for Funding Advantage & Individual Advantage
>
- Explanation of Benefits for Funding Advantage Members
- Member FAQs
- Member-Hybrid >
- Member-Traditional >
- Member-Essentials >
- Member-PPO >
- Member-Cost Saver >
- Member-Minimum Essential Coverage >
- Member - Community Health Plan >
- Member-H&H PLan >
- Member-Vault PPO Resources >
- Member-Vault RBP >
- Member-Fundamental Care
- Member-Fundamental Care Value Plan
- Member Resources for Individual Advantage
- Benefit Extras >
- Self-Service Login >
- Find A Provider
- Prescription Benefits
- Member Download Forms >
-
Member Resources for Funding Advantage & Individual Advantage
>
-
Agents
- Provider
- About Us
- Contact Us









 RSS Feed
RSS Feed